
SuperTy’s Timeline – Our Cancer Story
We call him SuperTy for a reason. Over the course of two years and two months, SuperTy endured 20 surgeries, 11 cycles of various chemotherapies, 44 rounds of radiation to the brain and brainstem and 60 two-hour treatments in a state-of-the-art hyperbaric oxygen chamber. One year after radiation therapy was completed, Ty suffered a brain bleed and brainstem necrosis that left him paralyzed from head-to-toe. He had severe infections of the central nervous system four times throughout treatment, including MRSA meningitis, MSSA meningitis and fungal (Candida) meningitis. He experienced chronic hydrocephalus on and off for two years, resulting in severe pain and a multitude of shunt problems. He spent more than 225 nights in a hospital bed. Despite all of this, he never stopped fighting and he never stopped smiling every step of the way. Ty Campbell was indeed “super” in every way.
- Aug. 2010
- Sept. 2010
- Oct. 2010
- Nov. 2010
- Dec. 2010
- Jan. 2011
- Feb. 2011
- Mar. 2011
- Apr. 2011
- May 2011
- June 2011
- July 2011
- Aug. 2011
- Sept. 2011
- Oct. 2011
- Nov. 2011
- Dec. 2011
- Jan. 2012
- Feb. 2012
- Mar. 2012
- Apr. 2012
- May 2012
- June 2012
- July 2012
- Aug. 2012
- Sept. 2012
- Oct. 2012
-

Aug. 2010
Ty is admitted to Cohen’s Children’s Hospital with headaches.
Ty is diagnosed with a mass at the base of his skull, pressing against his brainstem. We go home.
The majority of the tumor is removed via endoscopic brain surgery performed through his nose and mouth.
Follow-up surgery is required to patch a hole in the dura/stop a serious CSF leak resulting from the first surgery. Ty’s first VP shunt is also added to replace a temporary lumbar drain.
Ty pulls out his NG tube out of frustration and discomfort (neo-gastral feeding tube that was placed in the nose). TPN begins and we discuss whether or not a g-tube would be required.
-

Sept. 2010
MRSA meningitis is confirmed. A PICC line is surgically placed in Ty’s arm.
A very anxious Ty pulls his PICC line out of his arm. Ty’s final pathology comes back declaring his tumor an extra-renal rhabdoid tumor.
Two more procedures are performed in the OR. Ty comes back with a feeding tube in his belly (G-tube) and a central line under his clavicle (soon to be replaced by a mediport).
After 27 nights, Ty goes home to rest before starting chemo at Memorial Sloan Kettering Cancer Center.
-
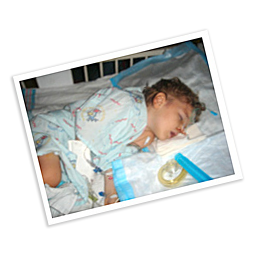
Oct. 2010
Surgery to place a double-lumen mediport under his shoulder. First round of HD-CAV chemotherapy begins that same day (high-dose cyclophosphamide, docorubicin and vincristine).
Ty suffers a stroke-like episode that causes another type of meningitis (non-bacterial). An MRI reveals that his tumor appears to be growing rapidly despite having chemo on-board. We are told to prepare for the worst.
Subsequent radiology reports determine that the tumor was hemmoraging rather than growing, a good sign of effective chemotherapy cutting off blood supply. We celebrate and rejoice. Hallelujah!
Ty has a short break from the hospital to recover and go Trick-or-Treating. Halloween is the last time he’s strong enough to stand on his own.
-
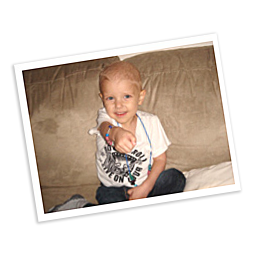
Nov. 2010
Round 2 of HD-CAV chemotherapy begins with 2 days of infusions.
Ty is taken off the IV antibiotics he was taking every six hours for the first time since he was diagnosed with MRSA in August. This was a double-edged sword. We knew we would have to take him off the antibiotics at some point, but feared the possibility of a shunt infection.
Back in the hospital – neutropenic with fever.
Ty is diagnosed with a fungal meningitis (Candida). His shunt is now certainly infected.
Surgery is performed to remove his shunt and place an externalized CSF drain until infection clears.
Ty receives a new VP shunt (his second). A post-surgical scan shows a film and several new lesions growing around his spinal cord - the first sign that Ty’s cancer has spread.
-

Dec. 2010
A series of follow-up MRIs show three new tumors on his spinal cord. He is diagnosed with lepto-meningial disease and we are told at the rate his cancer is spreading, he may have as little as four weeks left to live. At-home hospice care is arranged. Our hearts break into a million pieces but we hold onto hope.
Make A Wish sends us to DisneyWorld.
Ty is scheduled to begin full cranio-spinal radiation as a palliative measure, but we request an MRI beforehand to see how much the disease has progressed. The MRI results are somewhat confusing, so radiation is put on hold another week.
-
Jan. 2011
Ty is still doing well, and the disease on his latest MRI doesn’t appear to be progressing. His doctors are confused and a small debate arises as to whether or not they could have been mistaken about the lepto-menigial disease. It’s impossible to prove, so we are forced to wait and see.
A subsequent MRI reveals that the new lesions on the spinal cord are shrinking without explanation. A true miracle, thanks be to God!!
Ty is rushed to the hospital practically unconscious. His shunt was malfunctioning and needed to be replaced immediately. This is his third shunt revision. Chemotherapy remains on hold because of the poor condition of his bone marrow (among other issues).
-
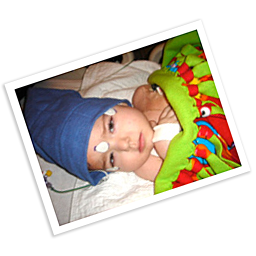
Feb. 2011
Another emergency trip to the hospital. Ty loses his ability to speak and quickly becomes unresponsive. CT and MRI show that his original tumor is growing rapidly on his brainstem. High-dose steroids save his life. We are told that he won’t survive another day or two and our only option other than giving up is to consider having the tumor removed surgically.
Surgery is performed to remove VP shunt and create a “map” of the tumor/brainstem in preparation for second tumor resection.
Ty has a craniotomy to remove the tumor. Most of the tumor on the brainstem is removed, with some disease remaining on the wall of the brainstem that will be treated with radiation.
Surgery to replace Ty’s VP shunt is performed (his fourth shunt).
-
Mar. 2011
Ty begins radiation therapy at Sloan Kettering (IMRT). He is scheduled for 30 treatments over a six week period. At this point, Ty is suffering from complete steroid myopathy. He can’t move his legs and he is limited to only slight movement of his right arm.
Ty is admitted to the PICU due to extreme pain and lethargy. An EEG is performed. No seizures., thank God. Not sure what’s wrong yet.
Feeling better, we are discharged.
Fever. We are re-admitted after Ty’s morning radiation treatment. We begin weening him off the steroids.
Another bacterial infection is found in Ty’s CSF. Intrathecal antibiotic injections are given daily, directly into Ty’s shunt, to try and put off another surgical shunt revision until after radiation therapy is completed.
-
April 2011
Ty is finally discharged again. Daily radiation therapy continues.
Back in the hospital to manage symptoms from potential infection.
Ty has his final radiation treatment to the brainstem area. As a result of severe head pain and vomiting, an MRI is scheduled. Two new lesions are discovered in Ty’s Cerabellum that same day. We are discharged.
-

May 2011
Ty can move his left arm! He is slowly recovering from the steroid myopathy since being weened off.
Ty begins his first cycle of Cisplatin (chemotherapy via infusion) and undergoes another surgery to externalize his VP drain and clear his CNS of infection before replacing it.
Surgery to place a new VP shunt (his fifth).
-

June 2011
Ty begins second cycle of Cisplatin and we add Temodar to the treatment as well.
Ty is rushed to the hospital. He is showing severe neurological symptoms. A follow-up scan shows that the Cerabellum tumors have tripled in size despite the chemotherapy. Steroids begin again. We beg for options.
Ty undergoes another craniotomy to remove the tumors in his Cerabellum. Surgery is 100% successful.
Surgical debris causes a clog in Ty’s VP shunt. Another surgery is required to fix the issue (Ty’s sixth shunt surgery). Ty’s eyes are severely crossed as a result (but they slowly get better after surgery)
-
July 2011
Ty begins another three week course of radiation therapy. 15 treatments of traditional radiation therapy to the Cerabellum area.
Ty receives his first course of a new chemotherapy – Avastin.
Family vacation in Schroon Lake.
-
Aug. 2011
Ty’s one-year anniversary since diagnosis.365 days of cancer.
We switch to a metronomic chemotherapy regimen, beginning with a 21-day cycle of Temodar paired with Celebrex.
-

Sept. 2011
Ty begins PT, OT and speech at home. We enroll him in a preschool program.
-
Oct. 2011
Ty turns four!! Daily chemo continues. All is good in the world.
-

Nov. 2011
Lou runs NYC marathon for Fred’s team. We take a family vacation in Mexico. These were the best days of our lives.
-

Dec. 2011
Ty suffers a significant post-radiation bleed at the brainstem. He suffers weakness throughout the left side of his body.
Ty’s bi-monthly MRI confirms that what we are seeing is more likely treatment effect in the brainstem area, as opposed to disease. Ty should be able to recover over time.
-
Jan. 2012
Avastin is on hold for a month so Ty’s platelets can be monitored more closely after the recent brain bleed.
Ty has a round of steroids to reduce brainstem swelling.
MRI shows NED.
We return to the hospital because Ty is showing incontinence and other signs of hydrocephalus. His shunt needed to be reprogrammed after the MRI earlier that week.
-
Feb. 2012
Ty reaches 13 kilos again for the first time since he was diagnosed 18 months prior. At his lowest, he weighed only 10 Kilos in May 2011.
Bi-monthly MRI shows no evidence of disease.
-

Mar. 2012
We return to the hospital. Something is wrong with Ty. We are inpatient for cultures and monitoring. A virus is suspected.
Ty is feeling a little better, and we go home to recoup.
Ty regresses and we check back into the hospital. Just two days later, he loses the ability to move his arms and legs overnight.
A repeat MRI shows the possible cause to be necrosis in the brainstem. An after-effect from the radiation therapy that was completed a year ago. Necrosis is potentially fatal.
-
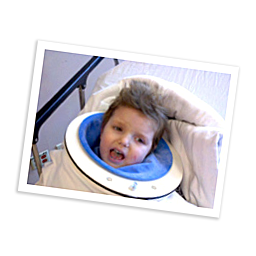
Apr. 2012
Ty stabilizes and he transfers to another facility (Blythedale Children’s Hospital) for inpatient physical therapy.
Ty has tubes placed in his ears in order to receive hyperbaric oxygen therapy. A minor outpatient procedure, still – it marks Ty’s 17th surgery.
Ty goes into the hyperbaric oxygen chamber (HBO) for the first time. He is scheduled to receive daily 90-minute treatments for the next 30 – 60 days.
-

May 2012
We finally go home. Ty’s therapy is switched to an outpatient program at Blythedale, and HBO treatments continue each morning.
Ty’s bi-monthly MRI (full brain and spine) shows improvement in the brainstem area and no evidence of disease. This gives us hope for his eventual physical recovery.
Emergency shunt surgery is performed. The tubing connecting the valve to the brain is clogged and Ty suffers from hydrocephalus. This marks his 7th shunt revision, and his 18th surgery.
Ty has 102 fever and is recovering in the PICU.
Ty is discharged. Resumes daily chemotherapy regimen. Returns to daily HBO treatments and physical therapy routine.
-
June 2012
Daily chemo and oxygen therapies continue.
Ty has sporadic head pain and vomiting but MRI of the brain shows NED.
The Campbell’s take a two week vacation in Long Beach. In the middle of those two weeks, Ty is rushed to MSKCC for yet another shunt revision (shunt surgery #8 in 18 months). This marks Ty’s 19th surgery in less than two years.
Ty recovers wonderfully and finishes off his vacation with a smile.

July 2012
Ty completes outpatient treatment at Blythdale Children’s hospital following approval from the school district to reinstate at-home therapies.
The Ty Louis Campbell Foundation participates in its first athletic fundraiser (5K) for the Children’s Brain Tumor Project at Weill Cornell and raises over $15,000.
Ty’s gastronomy tube is accidentally pulled out while at home. Thank God for our neighbor who happens to be an oncology nurse!
-
Aug. 2012
We “celebrate” Ty’s two-year anniversary since his diagnosis on August 11, 2010.
Team SuperTy bikes 168 miles in two days to complete the renowned Pan Mass challenge – raising thousands of dollars for cancer research at the Dana Farber institute.
Ty’s completes his last treatment in the hyperbaric oxygen chamber. He has a total of 60 sessions under his belt by this time. Each session takes about 2 hours.
Team SuperTy is at it again. Participants in “Swim Across America” raise thousands of dollars for Memorial Sloan Kettering.
-

Sept. 2012
Ty’s doctors examine a small wound that is beginning to spread right where the valve of his shunt it. The hardware may have been exposed. Another shunt replacement is required. This marks his 20th surgery, and his 9th shunt revision.
Ty has increased secretions post-surgery. He seems to be having a lot of trouble swallowing.
Ty is rushed to the hospital and shows signs of hydrocephalus that is later confirmed by CT. Shunt malfunction is likely, however we insist on an MRI before making any decisions on another surgery.
The MRI shows progressive, metastatic disease. Ty is diagnosed with lepto-meningial enhancement. He is sent home on hospice care on Sept. 17. To say our hearts are broken is an extreme understatement.
-

Oct. 2012
Ty turns 5 years old on October 4th. We are in awe of his strength.
Team SuperTy, once again, runs a 13K in Prospect Park and donates almost $15,000 to the Children’s Brain Tumor Project at Weill Cornell.
After more than three weeks on hospice care at-home, Ty is still smiling every single day but he also begins to grow more tired.
Ty spikes a very high fever out of nowhere on October 15th. It is somewhat controlled by Tylenol. He falls into a heavy sleeping pattern and is barely aroused.
Around 2PM on October 17th, Ty wakes up briefly to say goodbye to his Mommy and Daddy. He takes his last breath in their arms. A void consumes our hearts and a chronic lump develops in our throats. Once again, our lives are forever changed.
After fighting valiantly for half his life, Ty finally beat cancer once and for all when he became a beloved angel on October 17, 2012.
Where It All Began
Ty Louis Campbell was our little fighter. He was diagnosed with a malignant rhabdoid tumor at the base of his skull in August 2010. He was two years and ten months old. His story is one that is filled with tragedy and triumph.
Ty was a rambunctious toddler with curly blonde hair and an infectious smile. He didn’t have any developmental delays, medical issues or neurological deficits prior to his diagnosis. However, Ty was never a good sleeper since the day he was born. He woke up frequently throughout the night crying and whining, but we could always soothe him back to sleep. We discussed this with his pediatrician on several occasions and finally decided to schedule a sleep study for some time in late August 2010. Days after scheduling that appointment, we experienced a week straight of increasingly sleepless nights and decided to instead take him to the emergency room for imaging. He was crying and whining all through the night but he couldn’t tell us why and we just couldn’t stand it anymore.
Ty didn’t have any neurological symptoms. The doctor’s at Cohen’s Children’s Hospital (Long Island, NY) didn’t seem very concerned, but they reassured us that it was a good idea to get an MRI just in case. Since his case wasn’t urgent, we had to stay overnight inpatient because we were waiting for MRI/anesthesia availability. Ty slept beautifully at the hospital. Not even a whimper all night. We laughed the next morning and couldn’t wait to get the MRI over with so we could go home looking like silly, worried parents. At least we would be at peace knowing that he was fine.
We packed up our things and waited anxiously to go home. Ty’s Daddy, Lou, was standing in the hallway when he saw the neurology team heading down toward our room. “Is it good? Can we go?” he asked with a smile. “No?” With that he turned to look at me and the walls around us began the melt. The sounds in the room became amplified and muffled. The world around us was falling to pieces.
The MRI image showed Ty’s profile with a tumor, about one inch in diameter, growing from his clivis (the base of his skull behind the nose) and pushing against his brainstem. No wonder he couldn’t sleep. Lying down increased the pressure on his brainstem and was causing intermittent head pain.
The following week was a blur. We traveled to speak with several of the nation’s best pediatric neuro-surgeons. We talked about the different approaches which ranged from cutting through his upper jaw (also known as a La Forte) to trying an endoscopic approach through his nose and mouth. We spoke to strangers who had children going through similar surgeries. We answered every phone call and followed through on countless recommendations (…”you must talk to this doctor… you must look into this facility… you must feed him apricot seeds…etc.”).
During this short week at home, Ty began to fall apart before our eyes. It was as if the tumor decided to come out of hiding. Ty’s speech began to slur. He lost the ability to drink from a straw, then from a sippy cup. His head pain was becoming unbearable and he started suffering during the daytime, too. We went home with a smiling toddler and were told to take our time deciding on surgery. Instead we had to rush him into surgery just days later. 90% of the tumor was successfully removed endoscopically through his nose and mouth – an innovative approach.
And so our journey began. Listed below is a chronicle of our little fighter’s battle with cancer. We hope you will continue to follow our family’s journey on www.superty.org and like him on Facebook at www.facebook.com/thelittlefighter. We believe he found his strength from the support of so many friends and strangers. A fighter he was, indeed.
Ty’s Mommy






